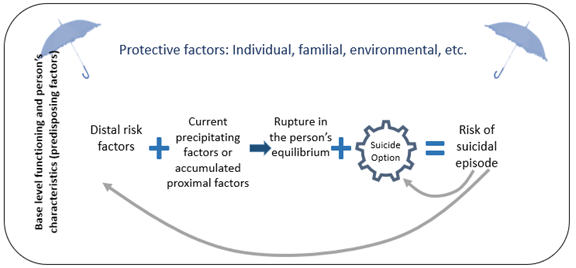
The dynamic model of suicide presents the development of suicide risk in persons with ID or ASD. It aims to support the professionals in understanding suicide risk as a process that is dynamic, multifactorial and that evolves with time.
It falls within the diathesis-stress models of suicide.
Suicide risk: the result of multiple factors in interaction
In the dynamic model of suicide described in the IDAS Process, the suicide risk in persons with an ID or ASD is the consequence of an interaction between:
- Predisposing factors in base level functioning and individual characteristics (ex.: cognitive rigidity, communication skills, socioeconomic level, etc.) and risk factors (ex.: experiences of abuse or family violence, mental health, recurring conflicts, etc.)
- Critical moments and precipitating factors, either one-time (ex.: conflict, breakup) or recurrent with a cumulative effect (ex.: multiples experiences of unremarkable rejection).
Such a combination can provoke a rupture in the person’s emotional and cognitive equilibrium.
When the suicide option is present, there is a risk of suicidal episode. The model also considers the presence of protective factors. These act as a counterweight, at different levels of the suicidal process, to reduce the risk of a suicidal episode.
Each experience of a suicidal episode increases suicide risk, since past suicidal behavior is a major suicide risk factor. Therefore, the suicide option is reinforced through every suicidal episode.
| The IDAS Process cannot replace clinical judgement. It aims to support and complement it. It constitutes a framework for identifying relevant information and guide the clinical decision-making on the level of danger and on the adequate interventions to put in place. |
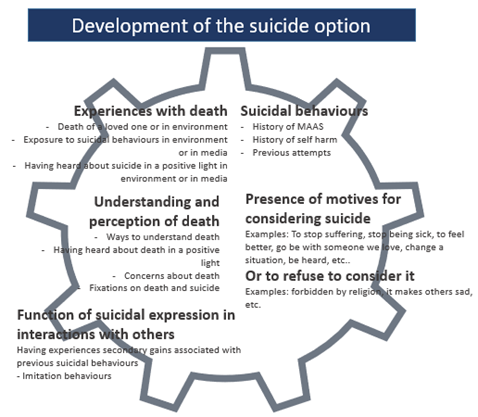
Development of the suicide option
Development of the suicide option refers to suicide becoming a possible solution to problems for an individual. It can develop in various ways but includes at least on element described in the adjacent Figure.
Development of the suicide option is at the centre of the dynamic model of suicide described in the IDAS Process.
For more details, see Practical foundations of the IDAS Process and general structure
Manifestations associées au suicide (suicide-related manifestations)
The term “Manifestations associées au suicide” (MAAS) – or suicide-related manifestations – was chosen to reflect the variety of verbal, non-verbal, direct and indirect behaviours that can express suicidality in people with ID or ASD.
| Type of MAAS | Examples of suicide-related manifestations |
| Thoughts (unobservable or not communicated) | Thinking about their own death when they are sad Thinking about hiding a knife in their room Having suicidal flashes or seeing themselves dead Thinking about the reaction of loved ones if they were dead or missing |
| Direct verbal communications | “I want to die”; “I want to kill myself”; “I have dark thoughts”. |
| Indirect verbal communications | “I want to join my grandmother at the cemetery”; “I would like to be dead”; “You would be better off without me”; “I want to go far and not come back”; “I want to go with the birds”; “I want to act like … (the person who killed himself)” |
| Direct or indirect verbal communications by text or social media | In the form of sentences (statements, questions), images, ‘’likes’’ on posts about death or suicide, etc. |
| Non-verbal communications | Drawings representing a violent act or a suicidal gesture, graves, suffering, objects to commit suicide Miming strangling themselves, cutting themselves |
| Self-aggressive behaviours without injury | Trying to push a non-cutting object (a branch) through the skin (in the stomach, arm or leg) Swallowing pills or non-toxic substances (without knowing the level of danger) Trying to strangle themselves with their hands or holding their breath |
| Self-aggressive behaviours with injury or death | Swallowing pills or substances with toxic potential (drugs) Injuring themselves with a sharp object Strangling or hanging themselves with a belt, towel, or rope Jumping from a window or from a high place Jumping in front of a vehicle Jumping into the water (without knowing how to swim, without looking) Crossing the street on a red light or a metro rail |
| Signs associated with MAAS
These clues can help identify a person at risk who does not verbally express distress and suicidal ideation |
Cognitive: confusion, difficulty concentrating, indecision Emotional: mood swings, manifestations of sadness, anger, irritability, increased anxiety about upcoming events, anxiety, increased aggressiveness, dissatisfaction, disappointment, fears or insecurity in the face of a situation, feeling of incompetence Psychiatric: increased symptoms Losses in acquired capabilities and adaptation difficulties in the current situation: stagnation or regression Behavioural: behaviour changes (worse or better, agitation or prostration, amplification of usual challenging behaviours, increased substance use or compulsive behaviour, isolation, increased request for help, absenteeism) Somatic: emergence or worsening of physical and digestive disorders, back pain, headaches, etc. Neuro-vegetative: deterioration of sleep, appetite, energy level Signs of hopelessness: negative discourse about the future, discouragement, resignation, self-deprecation, cessation of treatment, refusal of follow-up or absences, refusal of the help offered |
